Nerve Pain Between the Toes
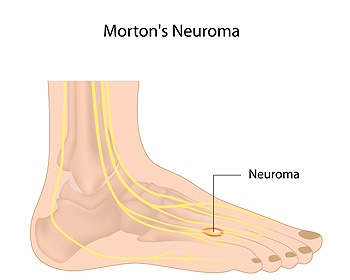
Morton’s neuroma is caused by irritation or damage to a nerve in the foot. It typically affects the nerve between the third and fourth toes and causes a shooting, stabbing, or burning pain, as well as an odd sensation of walking on a pebble. Morton’s neuroma can also cause tingling and numbness in the foot. Symptoms may get worse while moving your foot, bearing weight, or wearing high heels or tight shoes. This condition tends to worsen without treatment. If you are suffering from pain in the ball of the foot, it is suggested that you seek the care of a podiatrist.
Morton’s neuroma is a very uncomfortable condition to live with. If you think you have Morton’s neuroma, contact Dr. Joshua David Scoll of Pennsylvania. Our doctor will attend to all of your foot care needs and answer any of your related questions.
Morton’s Neuroma
Morton's neuroma is a painful foot condition that commonly affects the areas between the second and third or third and fourth toe, although other areas of the foot are also susceptible. Morton’s neuroma is caused by an inflamed nerve in the foot that is being squeezed and aggravated by surrounding bones.
What Increases the Chances of Having Morton’s Neuroma?
- Ill-fitting high heels or shoes that add pressure to the toe or foot
- Jogging, running or any sport that involves constant impact to the foot
- Flat feet, bunions, and any other foot deformities
Morton’s neuroma is a very treatable condition. Orthotics and shoe inserts can often be used to alleviate the pain on the forefront of the feet. In more severe cases, corticosteroids can also be prescribed. In order to figure out the best treatment for your neuroma, it’s recommended to seek the care of a podiatrist who can diagnose your condition and provide different treatment options.
If you have any questions, please feel free to contact one of our offices located in Philadelphia, Bensalem, and Fairless Hills, PA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Why a Podiatrist Can Be a Pregnant Woman’s Best Friend
Everything swells when you are pregnant, and your feet and ankles are no exception. This swelling (edema) during pregnancy is caused when your body produces and retains more blood and fluids to feed the growing baby in your uterus. The inordinate amount of pressure that the uterus places on blood vessels causes them to struggle with pumping blood back out of your feet and legs. Also, the extra fluids your body creates during pregnancy tend to gather in the lower extremities during the day when you are standing and sitting. You can help ease the symptoms of edema by wearing comfortable shoes, drinking plenty of water, and taking breaks to elevate and stretch your feet throughout the day. The stress and strain of extra weight and swelling can lead to other conditions in your feet such as corns, calluses, pain, and overpronation—where the foot flattens and rolls inwardly while walking. A podiatrist is an important part of a woman’s medical team during pregnancy. They can give professional advice on exercises and footwear, treat uncomfortable foot and ankle conditions, and prescribe custom orthotics to help ease pain and distribute excess weight more evenly across the feet.
Pregnant women with swollen feet can be treated with a variety of different methods that are readily available. For more information about other cures for swollen feet during pregnancy, consult with Dr. Joshua David Scoll from Pennsylvania. Our doctor will attend to all of your foot and ankle needs.
What Foot Problems Can Arise During Pregnancy?
One problem that can occur is overpronation, which occurs when the arch of the foot flattens and tends to roll inward. This can cause pain and discomfort in your heels while you’re walking or even just standing up, trying to support your baby.
Another problem is edema, or swelling in the extremities. This often affects the feet during pregnancy but tends to occur in the later stages.
How Can I Keep My Feet Healthy During Pregnancy?
- Wearing orthotics can provide extra support for the feet and help distribute weight evenly
- Minimize the amount of time spent walking barefoot
- Wear shoes with good arch support
- Wear shoes that allow for good circulation to the feet
- Elevate feet if you experience swelling
- Massage your feet
- Get regular, light exercise, such as walking, to promote blood circulation to the feet
If you have any questions please feel free to contact one of our offices located in Philadelphia, Bensalem, and Fairless Hills, PA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
The Basics of Diabetic Foot Care
If you or someone you take care of has diabetes, there are a number of preventative practices that should be implemented to help keep your feet healthy and to avoid serious complications down the road. Shoes and socks should be worn during waking hours, even around the house. Check to make sure shoes fit properly and that there are no rough edges that will scrape against or cause a disturbance in the skin. Examine the feet daily. Early detection of any break in the skin will help avoid the injury from developing into a wound. Keep the feet clean and dry and the toenails trimmed straight across. Toenail length should be level with the tips of the toes, but not too short in order to prevent the nail from growing into the skin. Finally, any diabetic should be under the care of a podiatrist who can help them maintain proper foot health and manage any complications should they arise.
Diabetic foot care is important in preventing foot ailments such as ulcers. If you are suffering from diabetes or have any other concerns about your feet, contact Dr. Joshua David Scoll from Pennsylvania. Our doctor can provide the care you need to keep you pain-free and on your feet.
Diabetic Foot Care
Diabetes affects millions of people every year. The condition can damage blood vessels in many parts of the body, especially the feet. Because of this, taking care of your feet is essential if you have diabetes, and having a podiatrist help monitor your foot health is highly recommended.
The Importance of Caring for Your Feet
- Routinely inspect your feet for bruises or sores.
- Wear socks that fit your feet comfortably.
- Wear comfortable shoes that provide adequate support.
Patients with diabetes should have their doctor monitor their blood levels, as blood sugar levels play such a huge role in diabetic care. Monitoring these levels on a regular basis is highly advised.
It is always best to inform your healthcare professional of any concerns you may have regarding your feet, especially for diabetic patients. Early treatment and routine foot examinations are keys to maintaining proper health, especially because severe complications can arise if proper treatment is not applied.
If you have any questions please feel free to contact one of our offices located in Philadelphia, Bensalem, and Fairless Hills, PA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Post-surgical Care For Ingrown Toenails
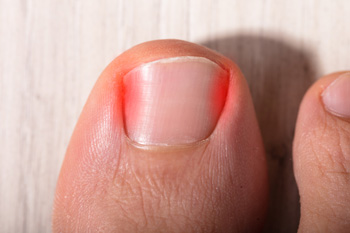
Ingrown toenails are nails whose edges that have grown into the surrounding skin. This may cause the area to become red, swollen, tender, and painful, and puts you at an increased risk of getting an infection. In severe cases, an ingrown toenail may need to be surgically removed. Following a surgery for ingrown toenails, you should rest and elevate the affected foot for 12 to 24 hours. Over the counter medications can be used to manage pain. Two days after your surgery, you can begin to soak your foot in warm, soapy water several times a day. Following the soak, apply an antibiotic ointment and cover the area with a clean bandage. For more information about treatments for ingrown toenails, please consult with a podiatrist.
Ingrown toenails can become painful if they are not treated properly. For more information about ingrown toenails, contact Dr. Joshua David Scoll of Pennsylvania. Our doctor can provide the care you need to keep you pain-free and on your feet.
Ingrown Toenails
Ingrown toenails occur when a toenail grows sideways into the bed of the nail, causing pain, swelling, and possibly infection.
Causes
- Bacterial infections
- Improper nail cutting such as cutting it too short or not straight across
- Trauma to the toe, such as stubbing, which causes the nail to grow back irregularly
- Ill-fitting shoes that bunch the toes too close together
- Genetic predisposition
Prevention
Because ingrown toenails are not something found outside of shoe-wearing cultures, going barefoot as often as possible will decrease the likeliness of developing ingrown toenails. Wearing proper fitting shoes and using proper cutting techniques will also help decrease your risk of developing ingrown toenails.
Treatment
Ingrown toenails are a very treatable foot condition. In minor cases, soaking the affected area in salt or antibacterial soaps will not only help with the ingrown nail itself, but also help prevent any infections from occurring. In more severe cases, surgery is an option. In either case, speaking to your podiatrist about this condition will help you get a better understanding of specific treatment options that are right for you.
If you have any questions please feel free to contact one of our offices located in Philadelphia, Bensalem, and Fairless Hills, PA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Signs of RA in the Feet and Ankles
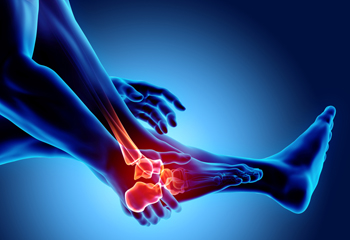 Rheumatoid arthritis (RA) is an autoimmune disease that causes the body’s immune system to attack otherwise healthy cells in the lining of the joints. The joints become inflamed, leading to pain, swelling, stiffness, redness, and warmth. RA frequently affects the small joints of the feet and the ankle joints. Many foot conditions are related to RA, including dislocated toe joints, hammertoes, bunions, heel pain, Achilles tendonitis, flat foot, and ankle pain. People with RA can also develop rheumatoid nodules, lumps on the feet that can cause pain while walking or when they rub against the shoes. If you have RA, a podiatrist can help you manage this condition and maintain the proper health of your feet.
Rheumatoid arthritis (RA) is an autoimmune disease that causes the body’s immune system to attack otherwise healthy cells in the lining of the joints. The joints become inflamed, leading to pain, swelling, stiffness, redness, and warmth. RA frequently affects the small joints of the feet and the ankle joints. Many foot conditions are related to RA, including dislocated toe joints, hammertoes, bunions, heel pain, Achilles tendonitis, flat foot, and ankle pain. People with RA can also develop rheumatoid nodules, lumps on the feet that can cause pain while walking or when they rub against the shoes. If you have RA, a podiatrist can help you manage this condition and maintain the proper health of your feet.
Because RA affects more than just your joints, including the joints in your feet and ankles, it is important to seek early diagnosis from your podiatrist if you feel like the pain in your feet might be caused by RA. For more information, contact Dr. Joshua David Scoll of Pennsylvania. Our doctor will assist you with all of your podiatric concerns.
What Is Rheumatoid Arthritis?
Rheumatoid Arthritis (RA) is an autoimmune disorder in which the body’s own immune system attacks the membranes surrounding the joints. Inflammation of the lining and eventually the destruction of the joint’s cartilage and bone occur, causing severe pain and immobility.
Rheumatoid Arthritis of the Feet
Although RA usually attacks multiple bones and joints throughout the entire body, almost 90 percent of cases result in pain in the foot or ankle area.
Symptoms
- Swelling and pain in the feet
- Stiffness in the feet
- Pain on the ball or sole of feet
- Joint shift and deformation
Diagnosis
Quick diagnosis of RA in the feet is important so that the podiatrist can treat the area effectively. Your doctor will ask you about your medical history, occupation, and lifestyle to determine the origin of the condition. Rheumatoid Factor tests help to determine if someone is affected by the disease.
If you have any questions please feel free to contact one of our offices located in Philadelphia, Bensalem, and Fairless Hills, PA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
What Is Sesamoiditis?
Sesamoid bones are connected to tendons instead of other bones or can be deeply embedded in muscle tissue. The largest sesamoid bone is the kneecap. Two other petite sesamoid bones, the size of corn kernels, are located at the base of the toe in the ball of the foot. When these bones become stressed due to overuse from activities such as ballet dancing, running, playing baseball or similar sports, the tendons surrounding the sesamoid bones become inflamed and painful. This is known as sesamoiditis. Check with a podiatrist if you suspect you are afflicted with sesamoiditis. Sometimes bruising can occur, and if it does it is normally mild. You can cushion the bruise with padding and avoid tight constricting shoes or other sources of friction. Podiatrists can help treat sesamoiditis with icing, compression bandages, and more, while prescribing rest and elevation of the affected foot.
Sesamoiditis is an unpleasant foot condition characterized by pain in the balls of the feet. If you think you’re struggling with sesamoiditis, contact Dr. Joshua David Scoll of Pennsylvania. Our doctor will treat your condition thoroughly and effectively.
Sesamoiditis
Sesamoiditis is a condition of the foot that affects the ball of the foot. It is more common in younger people than it is in older people. It can also occur with people who have begun a new exercise program, since their bodies are adjusting to the new physical regimen. Pain may also be caused by the inflammation of tendons surrounding the bones. It is important to seek treatment in its early stages because if you ignore the pain, this condition can lead to more serious problems such as severe irritation and bone fractures.
Causes of Sesamoiditis
- Sudden increase in activity
- Increase in physically strenuous movement without a proper warm up or build up
- Foot structure: those who have smaller, bonier feet or those with a high arch may be more susceptible
Treatment for sesamoiditis is non-invasive and simple. Doctors may recommend a strict rest period where the patient forgoes most physical activity. This will help give the patient time to heal their feet through limited activity. For serious cases, it is best to speak with your doctor to determine a treatment option that will help your specific needs.
If you have any questions please feel free to contact one of our offices located in Philadelphia, Bensalem, and Fairless Hills, PA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Cuboid Syndrome and Running
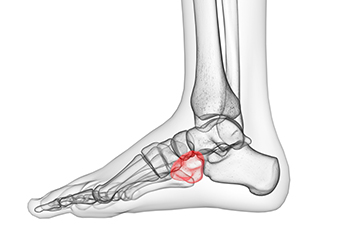 Cuboid syndrome is a condition in which the cuboid bone, located near the center of the foot, becomes displaced. If you’re a runner, this is a problem that you should watch out for. Your feet absorb shock up to two and a half times your body weight when you run. When all of the foot bones are properly aligned, your feet can absorb the shock without much discomfort. However, when the cuboid bone is displaced the feet can’t absorb shock as efficiently leading to foot pain, swelling, reduced range of motion, and difficulty bearing weight on the affected foot. Cuboid syndrome may occur in conjunction with an ankle sprain, or it can be caused by poor foot biomechanics or injury. If you are experiencing any foot pain please seek the care of a podiatrist.
Cuboid syndrome is a condition in which the cuboid bone, located near the center of the foot, becomes displaced. If you’re a runner, this is a problem that you should watch out for. Your feet absorb shock up to two and a half times your body weight when you run. When all of the foot bones are properly aligned, your feet can absorb the shock without much discomfort. However, when the cuboid bone is displaced the feet can’t absorb shock as efficiently leading to foot pain, swelling, reduced range of motion, and difficulty bearing weight on the affected foot. Cuboid syndrome may occur in conjunction with an ankle sprain, or it can be caused by poor foot biomechanics or injury. If you are experiencing any foot pain please seek the care of a podiatrist.
Cuboid syndrome, also known as cuboid subluxation, occurs when the joints and ligaments near the cuboid bone in the foot become torn. If you have cuboid syndrome, consult with Dr. Joshua David Scoll from Pennsylvania. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Cuboid syndrome is a common cause of lateral foot pain, which is pain on the outside of the foot. The condition may happen suddenly due to an ankle sprain, or it may develop slowly overtime from repetitive tension through the bone and surrounding structures.
Causes
The most common causes of cuboid syndrome include:
- Injury – The most common cause of this ailment is an ankle sprain.
- Repetitive Strain – Tension placed through the peroneus longus muscle from repetitive activities such as jumping and running may cause excessive traction on the bone causing it to sublux.
- Altered Foot Biomechanics – Most people suffering from cuboid subluxation have flat feet.
Symptoms
A common symptom of cuboid syndrome is pain along the outside of the foot which can be felt in the ankle and toes. This pain may create walking difficulties and may cause those with the condition to walk with a limp.
Diagnosis
Diagnosis of cuboid syndrome is often difficult, and it is often misdiagnosed. X-rays, MRIs and CT scans often fail to properly show the cuboid subluxation. Although there isn’t a specific test used to diagnose cuboid syndrome, your podiatrist will usually check if pain is felt while pressing firmly on the cuboid bone of your foot.
Treatment
Just as the range of causes varies widely, so do treatments. Some more common treatments are ice therapy, rest, exercise, taping, and orthotics.
If you have any questions, please feel free to contact one of our offices located in Philadelphia, Bensalem, and Fairless Hills, PA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Taking a Closer Look at Corns
Corns are hardened, thickened areas of skin on your feet that develop due to friction or pressure from footwear. They are typically small and round-shaped, getting their name from their similarity to a kernel of corn. Corns come in two varieties: hard and soft. Hard corns usually form on the tops of the toes and are dry and dense, while soft corns are found between the toes and have a more rubbery texture. Corns of any kind may cause pain or discomfort if there is pressure placed on them. Corns are particularly problematic, possibly leading to complications in people with diabetes or other conditions that affect blood flow to the feet. If you have developed a corn that is painful or chronic, or if you are a diabetic, please seek the professional care of a podiatrist.
Corns can make walking very painful and should be treated immediately. If you have questions regarding your feet and ankles, contact Dr. Joshua David Scoll of Pennsylvania. Our doctor will treat your foot and ankle needs.
Corns: What Are They? And How Do You Get Rid of Them?
Corns are thickened areas on the skin that can become painful. They are caused by excessive pressure and friction on the skin. Corns press into the deeper layers of the skin and are usually round in shape.
Ways to Prevent Corns
There are many ways to get rid of painful corns such as:
- Wearing properly fitting shoes that have been measured by a professional
- Wearing shoes that are not sharply pointed or have high heels
- Wearing only shoes that offer support
Treating Corns
Although most corns slowly disappear when the friction or pressure stops, this isn’t always the case. Consult with your podiatrist to determine the best treatment option for your case of corns.
If you have any questions please feel free to contact one of our offices located in Philadelphia, Bensalem, and Fairless Hills, PA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Can the Foods You Eat Affect Plantar Fasciitis?
Plantar Fasciitis is an inflammation of the band of tissue that connects your heel with your toes on the sole of your foot. Many people believe inflammation throughout the body can be reduced by making certain dietary adjustments—particularly by increasing the consumption of anti-inflammatory foods and decreasing consumption of inflammatory foods. Anti-inflammatory foods include green leafy vegetables, carrots, broccoli, strawberries, blueberries, tomatoes, legumes, nuts, lean meats, as well as tuna and salmon which are rich in omega-3 fatty acids. Inflammatory foods have high levels of sugar, including soft drinks, pastries and sweets, candy, processed foods, junk food, refined grains, as well as oils containing omega-6 fats (corn/soy/cottonseed oil), saturated fats and red meats. For more information on how to heal the pain and inflammation of plantar fasciitis, schedule an appointment with a podiatrist.
Plantar fasciitis is a common foot condition that is often caused by a strain injury. If you are experiencing heel pain or symptoms of plantar fasciitis, contact Dr. Joshua David Scoll from Pennsylvania. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is one of the most common causes of heel pain. The plantar fascia is a ligament that connects your heel to the front of your foot. When this ligament becomes inflamed, plantar fasciitis is the result. If you have plantar fasciitis you will have a stabbing pain that usually occurs with your first steps in the morning. As the day progresses and you walk around more, this pain will start to disappear, but it will return after long periods of standing or sitting.
What Causes Plantar Fasciitis?
- Excessive running
- Having high arches in your feet
- Other foot issues such as flat feet
- Pregnancy (due to the sudden weight gain)
- Being on your feet very often
There are some risk factors that may make you more likely to develop plantar fasciitis compared to others. The condition most commonly affects adults between the ages of 40 and 60. It also tends to affect people who are obese because the extra pounds result in extra stress being placed on the plantar fascia.
Prevention
- Take good care of your feet – Wear shoes that have good arch support and heel cushioning.
- Maintain a healthy weight
- If you are a runner, alternate running with other sports that won’t cause heel pain
There are a variety of treatment options available for plantar fasciitis along with the pain that accompanies it. Additionally, physical therapy is a very important component in the treatment process. It is important that you meet with your podiatrist to determine which treatment option is best for you.
If you have any questions, please feel free to contact one of our offices located in Philadelphia, Bensalem, and Fairless Hills, PA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
What Can Cause Heel Pain?
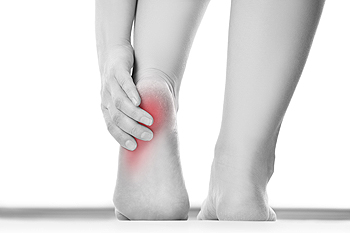 Heel pain can be debilitating for some patients, and can arise due to a variety of different causes. The three most common sources of heel pain are plantar fasciitis, Achilles tendonitis, and arthritis. Plantar fasciitis occurs when the plantar fascia, which is a band of tissue that runs along the bottom of the foot connecting the heel to the toes, becomes inflamed or torn. Achilles tendonitis is the result of the Achilles tendon, which connects the calf muscles to the heel bone, becoming inflamed. Other common causes of heel pain can include bursitis, stress fractures, or the wearing down of the heel pad at the bottom of the heel. If you are struggling with heel pain, consulting with a podiatrist for a proper diagnosis and treatment can be incredibly beneficial.
Heel pain can be debilitating for some patients, and can arise due to a variety of different causes. The three most common sources of heel pain are plantar fasciitis, Achilles tendonitis, and arthritis. Plantar fasciitis occurs when the plantar fascia, which is a band of tissue that runs along the bottom of the foot connecting the heel to the toes, becomes inflamed or torn. Achilles tendonitis is the result of the Achilles tendon, which connects the calf muscles to the heel bone, becoming inflamed. Other common causes of heel pain can include bursitis, stress fractures, or the wearing down of the heel pad at the bottom of the heel. If you are struggling with heel pain, consulting with a podiatrist for a proper diagnosis and treatment can be incredibly beneficial.
Many people suffer from bouts of heel pain. For more information, contact Dr. Joshua David Scoll of Pennsylvania. Our doctor can provide the care you need to keep you pain-free and on your feet.
Causes of Heel Pain
Heel pain is often associated with plantar fasciitis. The plantar fascia is a band of tissues that extends along the bottom of the foot. A rip or tear in this ligament can cause inflammation of the tissue.
Achilles tendonitis is another cause of heel pain. Inflammation of the Achilles tendon will cause pain from fractures and muscle tearing. Lack of flexibility is also another symptom.
Heel spurs are another cause of pain. When the tissues of the plantar fascia undergo a great deal of stress, it can lead to ligament separation from the heel bone, causing heel spurs.
Why Might Heel Pain Occur?
- Wearing ill-fitting shoes
- Wearing non-supportive shoes
- Weight change
- Excessive running
Treatments
Heel pain should be treated as soon as possible for immediate results. Keeping your feet in a stress-free environment will help. If you suffer from Achilles tendonitis or plantar fasciitis, applying ice will reduce the swelling. Stretching before an exercise like running will help the muscles. Using all these tips will help make heel pain a condition of the past.
If you have any questions please contact one of our offices located in Philadelphia, Bensalem, and Fairless Hills, PA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Sudden Ankle Pain May Be Due to Arthritis
If you suddenly experience ankle pain without any apparent reason or injury, it may have been brought on by some form of arthritis. For instance, osteoarthritis occurs when cartilage between bones wears down, causing them to rub together. This condition can sometimes cause sudden pain, often in the morning. Another type of arthritis—rheumatoid arthritis—causes your immune system to malfunction and attack healthy tissue. The lining in joints of the toes and ankles are a common location for rheumatoid arthritis to develop. A third type of arthritis that can affect your ankles is reactive arthritis. This occurs when a bacterial infection in another part of the body is responsible for generating arthritic symptoms like swelling and pain in your ankles. Gout is an arthritic condition caused by a build-up of uric acid in your body, which can crystallize on joints. Although gout typically affects the big toe, it can also develop in other joints, such as the ankle. Painful gout flare-ups are known to be intense and sudden, often occurring in the middle of the night. Pain of any kind in your ankles should prompt a visit to the podiatrist as soon as possible for an accurate diagnosis and treatment.
Ankle pain can be caused by a number of problems and may be potentially serious. If you have ankle pain, consult with Dr. Joshua David Scoll from Pennsylvania. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Ankle pain is any condition that causes pain in the ankle. Due to the fact that the ankle consists of tendons, muscles, bones, and ligaments, ankle pain can come from a number of different conditions.
Causes
The most common causes of ankle pain include:
- Types of arthritis (rheumatoid, osteoarthritis, and gout)
- Ankle sprains
- Broken ankles
- Achilles tendinitis
- Achilles tendon rupture
- Stress fractures
- Bursitis
- Tarsal tunnel syndrome
- Plantar fasciitis
Symptoms
Symptoms of ankle injury vary based upon the condition. Pain may include general pain and discomfort, swelling, aching, redness, bruising, burning or stabbing sensations, and/or loss of sensation.
Diagnosis
Due to the wide variety of potential causes of ankle pain, podiatrists will utilize a number of different methods to properly diagnose ankle pain. This can include asking for personal and family medical histories and of any recent injuries. Further diagnosis may include sensation tests, a physical examination, and potentially x-rays or other imaging tests.
Treatment
Just as the range of causes varies widely, so do treatments. Some more common treatments are rest, ice packs, keeping pressure off the foot, orthotics and braces, medication for inflammation and pain, and surgery.
If you have any questions, please feel free to contact one of our offices located in Philadelphia, Bensalem, and Fairless Hills, PA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
An Overview of Foot Pain
Pain can occur anywhere in the foot, and its location may be an indicator of the underlying condition. For instance, heel pain is very common and may be due to plantar fasciitis, Achilles tendinitis, injuries, or bone spurs. Pain in either the 2nd, 3rd, or 4th toes may emanate from a muscle imbalance, which eventually causes the toe to become bent in a downward position (hammertoe). Pain in one of the toe joints, the ankle joint, or the joint connecting the toes with the forefoot may be a warning sign of arthritis. Ingrown toenails can cause pain in, and on top of, the big toe. If you feel pain in the ball of your foot, it may be due to Morton’s neuroma—a thickening of tissue surrounding an irritated nerve between the toes. Arches may be painful due to wearing unsupportive shoes, having plantar fasciitis, or if the arches have fallen. Swollen or generally painful feet may be due to pregnancy, the heat, diabetes, or poor blood circulation. If you feel pain in any part of your feet, have a podiatrist perform an examination to diagnose your condition.
Foot Pain
Foot pain can be extremely painful and debilitating. If you have a foot pain, consult with Dr. Joshua David Scoll from Pennsylvania. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Causes
Foot pain is a very broad condition that could be caused by one or more ailments. The most common include:
- Bunions
- Hammertoes
- Plantar Fasciitis
- Bone Spurs
- Corns
- Tarsal Tunnel Syndrome
- Ingrown Toenails
- Arthritis (such as Gout, Rheumatoid, and Osteoarthritis)
- Flat Feet
- Injury (from stress fractures, broken toe, foot, ankle, Achilles tendon ruptures, and sprains)
- And more
Diagnosis
To figure out the cause of foot pain, podiatrists utilize several different methods. This can range from simple visual inspections and sensation tests to X-rays and MRI scans. Prior medical history, family medical history, and any recent physical traumatic events will all be taken into consideration for a proper diagnosis.
Treatment
Treatment depends upon the cause of the foot pain. Whether it is resting, staying off the foot, or having surgery; podiatrists have a number of treatment options available for foot pain.
If you have any questions, please feel free to contact one of our offices located in Philadelphia, Bensalem, and Fairless Hills, PA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
More...
Can Foot Wounds Be Prevented?
It is strongly suggested that diabetic patients do not ignore any signs of wounds developing on their feet. When there is prompt attention to cuts, sores, or bruises on the feet, symptoms like pain and discomfort may be avoided. Seeking treatment right away can also help prevent wounds from becoming infected; therefore, serious complications like amputation or gangrene can also be avoided. Gangrene destroys blood vessels and can block off blood flow due to swelling since diabetics already have a weakened immune system. It is imperative that existing foot wounds be cleaned daily with warm water, followed by covering them with a sterile bandage. Research has indicated that it can also be beneficial to wear shoes that fit properly as this may help in preventing painful foot wounds. If you are diabetic or you have developed a foot wound, please seek the care of a podiatrist who can help you manage this condition.
Wound care is an important part in dealing with diabetes. If you have diabetes and a foot wound or would like more information about wound care for diabetics, consult with Dr. Joshua David Scoll from Pennsylvania. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
What Is Wound Care?
Wound care is the practice of taking proper care of a wound. This can range from the smallest to the largest of wounds. While everyone can benefit from proper wound care, it is much more important for diabetics. Diabetics often suffer from poor blood circulation which causes wounds to heal much slower than they would in a non-diabetic.
What Is the Importance of Wound Care?
While it may not seem apparent with small ulcers on the foot, for diabetics, any size ulcer can become infected. Diabetics often also suffer from neuropathy, or nerve loss. This means they might not even feel when they have an ulcer on their foot. If the wound becomes severely infected, amputation may be necessary. Therefore, it is of the upmost importance to properly care for any and all foot wounds.
How to Care for Wounds
The best way to care for foot wounds is to prevent them. For diabetics, this means daily inspections of the feet for any signs of abnormalities or ulcers. It is also recommended to see a podiatrist several times a year for a foot inspection. If you do have an ulcer, run the wound under water to clear dirt from the wound; then apply antibiotic ointment to the wound and cover with a bandage. Bandages should be changed daily and keeping pressure off the wound is smart. It is advised to see a podiatrist, who can keep an eye on it.
If you have any questions, please feel free to contact one of our offices located in Philadelphia, Bensalem, and Fairless Hills, PA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
A Common Symptom of Tarsal Tunnel Syndrome
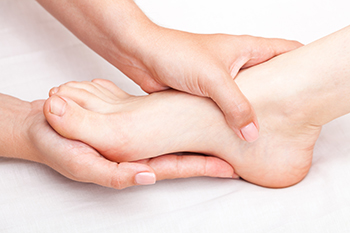 The tarsal tunnel is an area of the foot that is found below that ankle, and if it becomes inflamed as a result of an injury, tarsal tunnel syndrome may develop. This is caused by nerve that is located inside of the tarsal tunnel, called the tibial nerve, becoming pressed. A common symptom that is associated with this condition can consist of a burning sensation under the foot, and it could radiate to the toes and the heels. Walking may intensify this ailment, as it causes pressure to be put on the tibial nerve. If you have this type of pain, and it is hindering accomplishing daily activities, there are many options that are available for treatment. Please consult with a podiatrist who can recommend the best type of treatment for you.
The tarsal tunnel is an area of the foot that is found below that ankle, and if it becomes inflamed as a result of an injury, tarsal tunnel syndrome may develop. This is caused by nerve that is located inside of the tarsal tunnel, called the tibial nerve, becoming pressed. A common symptom that is associated with this condition can consist of a burning sensation under the foot, and it could radiate to the toes and the heels. Walking may intensify this ailment, as it causes pressure to be put on the tibial nerve. If you have this type of pain, and it is hindering accomplishing daily activities, there are many options that are available for treatment. Please consult with a podiatrist who can recommend the best type of treatment for you.
Tarsal tunnel syndrome can be very uncomfortable to live with. If you are experiencing tarsal tunnel syndrome, contact Dr. Joshua David Scoll of Pennsylvania. Our doctor can provide the care you need to keep you pain-free and on your feet.
Tarsal Tunnel Syndrome
Tarsal tunnel syndrome, which can also be called tibial nerve dysfunction, is an uncommon condition of misfiring peripheral nerves in the foot. The tibial nerve is the peripheral nerve in the leg responsible for sensation and movement of the foot and calf muscles. In tarsal tunnel syndrome, the tibial nerve is damaged, causing problems with movement and feeling in the foot of the affected leg.
Common Cause of Tarsal Tunnel Syndrome
- Involves pressure or an injury, direct pressure on the tibial nerve for an extended period of time, sometimes caused by other body structures close by or near the knee.
- Diseases that damage nerves, including diabetes, may cause tarsal tunnel syndrome.
- At times, tarsal tunnel syndrome can appear without an obvious cause in some cases.
The Effects of Tarsal Tunnel Syndrome
- Different sensations, an afflicted person may experience pain, tingling, burning or other unusual sensations in the foot of the affected leg.
- The foot muscles, toes and ankle become weaker, and curling your toes or flexing your foot can become difficult.
- If condition worsens, infections and ulcers may develop on the foot that is experiencing the syndrome.
A physical exam of the leg can help identify the presence of tarsal tunnel syndrome. Medical tests, such as a nerve biopsy, are also used to diagnose the condition. Patients may receive physical therapy and prescriptive medication. In extreme cases, some may require surgery.
If you have any questions please feel free to contact one of our offices located in Philadelphia, Bensalem, and Fairless Hills, PA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Helpful Tips for Measuring Your Feet
Planning a trip to the shoe store? Be sure to start with an accurate measurement to ensure you get shoes that are the right size. Start at the end of the day when your feet are at their largest, and stand up straight with one foot on a piece of paper (tape two pieces together if necessary). Carefully trace your foot’s shape with a pen or pencil held at a 90 degree angle. For the length: use a ruler or measuring tape to measure the tracing from the length of your foot from the bottom of your heel to the tip of the longest toe. To measure the width of your foot, wrap a measuring tape around the widest part of your foot (be sure you are pressing down the full weight of your body as you do it). Repeat the entire measuring process on your other foot. Check the largest measurements you’ve recorded against an online shoe size measurement tool to determine your ideal shoe size (length) and width (regular, wide, or extra wide). For more tips on choosing shoes most appropriate for your particular foot size and shape, consult with a podiatrist.
Getting the right shoe size is an important part of proper foot health. Seek the assistance of Dr. Joshua David Scoll from Pennsylvania. Our doctor will provide the care you need to keep you pain-free and on your feet.
Getting the Right Shoe Size
There are many people who wear shoes that are the incorrect size, negatively affecting their feet and posture. Selecting the right shoes is not a difficult process, so long as you keep several things in mind when it comes to choosing the right pair.
- When visiting the shoe store, use the tools available to measure your foot.
- Be sure there is ‘wiggle room’. There should be about an inch between your toes and the tip of your shoes.
- Do not always assume you are the same size, as manufacturers run differently.
- Purchase shoes later in the day, as your feet swell as the day progresses.
- If a shoe is not comfortable, it is not suitable. Most shoes can’t be ‘broken in’, and comfort should be the ultimate goal when it comes to choosing the right pair of shoes
As our feet hold our body weight and keep us moving, it is important to treat them right. Picking the right pair of shoes can provide your feet comfort and mobility without pain.
If you have any questions, please feel free to contact one of our offices located in Philadelphia, Bensalem, and Fairless Hills, PA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
What is an Acute Running Injury?
 Research has indicated that a staggering sixty percent of people who enjoy running have endured a running injury in the past year. These injuries may be the result of inconsistent training and possibly from increasing speed and distance too soon. An acute running injury is generally traumatic and happens suddenly. Now you're probably wondering what an acute running injury is. Most commonly they are strains and sprains, but can also be a muscle tear, bone crack, or ligament snap. Other running injuries may include plantar fascitiis, heel spurs, stress fractures, ankle sprains, and Achilles tendonitis. Whether a runner falls, twists an ankle, or gets struck by a vehicle, it's usually painful and associated with a "popping" sound followed by inflammation. Additionally, the foot may have a limited range of motion, and it may be difficult to walk. Runners may be able to prevent these injuries by paying attention to the type of ground they’re running on, being aware of their surroundings, and stretching before and after a run. There are many painful foot conditions that can occur from running injuries, and it is strongly suggested that you consult with a podiatrist who can provide helpful suggestions on how to prevent running injuries.
Research has indicated that a staggering sixty percent of people who enjoy running have endured a running injury in the past year. These injuries may be the result of inconsistent training and possibly from increasing speed and distance too soon. An acute running injury is generally traumatic and happens suddenly. Now you're probably wondering what an acute running injury is. Most commonly they are strains and sprains, but can also be a muscle tear, bone crack, or ligament snap. Other running injuries may include plantar fascitiis, heel spurs, stress fractures, ankle sprains, and Achilles tendonitis. Whether a runner falls, twists an ankle, or gets struck by a vehicle, it's usually painful and associated with a "popping" sound followed by inflammation. Additionally, the foot may have a limited range of motion, and it may be difficult to walk. Runners may be able to prevent these injuries by paying attention to the type of ground they’re running on, being aware of their surroundings, and stretching before and after a run. There are many painful foot conditions that can occur from running injuries, and it is strongly suggested that you consult with a podiatrist who can provide helpful suggestions on how to prevent running injuries.
All runners should take extra precaution when trying to avoid injury. If you have any concerns about your feet, contact Dr. Joshua David Scoll of Pennsylvania. Our doctor will treat your foot and ankle needs.
How to Prevent Running Injuries
There are a lot of mistakes a runner can make prior to a workout that can induce injury. A lot of athletes tend to overstretch before running, instead of saving those workouts for a post-run routine. Deep lunges and hand-to-toe hamstring pulls should be performed after a workout instead of during a warmup. Another common mistake is jumping into an intense routine before your body is physically prepared for it. You should try to ease your way into long-distance running instead of forcing yourself to rush into it.
More Tips for Preventing Injury
- Incorporate Strength Training into Workouts - This will help improve the body’s overall athleticism
- Improve and Maintain Your Flexibility – Stretching everyday will help improve overall performance
- “Warm Up” Before Running and “Cool Down” Afterward – A warm up of 5-10 minutes helps get rid of lactic acid in the muscles and prevents delayed muscle soreness
- Cross-Training is Crucial
- Wear Proper Running Shoes
- Have a Formal Gait Analysis – Poor biomechanics can easily cause injury
If you have any questions, please feel free to contact one of our offices located in Philadelphia, Bensalem, and Fairless Hills, PA . We offer the newest diagnostic and treatment technologies for all your foot care needs.