Heel Pain
Have you ever gotten up from a chair or out of bed in the morning, and upon taking that first step, feel like your heel has stepped on a tack? Many people experience a feeling of sharp pain which radiates into their arch from their heel and which does not allow them to put their heel on the floor. Sometimes they need to sit back down, stand only on their toes and use the wall for balance. If you can take a few steps, it seems to go away and lessen, allowing you to then resume your activity. Later, throughout your day and after a period of rest, it can happen again. If this sounds familiar you may be suffering from your first attack of heel pain.
Heel pain is a debilitating condition that affects day to day activities. Running and walking both causes stress on the heel because the heel is the part of the foot that hits the ground first. This means that the heel is taking on your entire weight. Diagnosis and treatments for heel pain can be easily found through your podiatrist.
Plantar Fasciitis
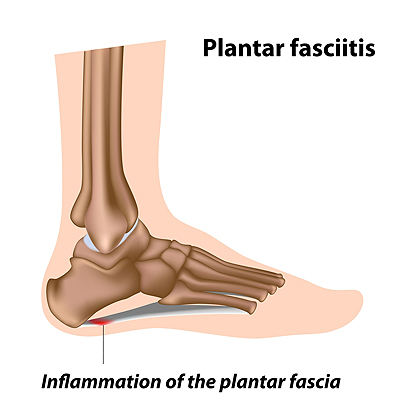
One of the main causes of heel pain is a condition known as plantar fasciitis. The plantar fascia is a band of tissue that extends along the bottom of the foot, from the toe to the bottom of the heel. A rip or tear in this ligament can cause inflammation of these tissues, resulting in heel pain. People who do not wear proper fitting shoes are often at risk of developing problems such as plantar fasciitis. Unnecessary stress from ill-fitting shoes, weight change, excessive running, and wearing non-supportive shoes on hard surfaces are all causes of plantar fasciitis.
Achilles Tendonitis
Achilles tendonitis is another cause of heel pain. Similar to plantar fasciitis, inflammation of the Achilles tendon will cause heel pain due to stress fractures and muscle tearing. A lack of flexibility of the ankle and heel is an indicator of Achilles tendonitis. If left untreated, this condition can lead to plantar fasciitis and cause even more pain on your heel.
Heel Spur
A third cause of heel pain is a heel spur. A heel spur occurs when the tissues of the plantar fascia undergo a great deal of stress, leading to a separation of the ligament from the heel bone entirely. This results in a pointed fragment of bone on the ball of the foot, known as a heel spur.
Matchmaker, Matchmaker, Make My Foot a Good Match
It is believed that many foot problems are caused by wearing the wrong kind of shoe. Here are some things you can do to help keep your feet healthy by choosing the right kind of shoe for your individual foot. Start by outlining your feet on a piece of paper and bringing that with you when you are buying shoes. Go in the afternoon or evening, after your foot has had a chance to expand throughout the day. When you get to the store, have your foot measured or do it yourself. Be sure to stand up to make sure each foot is measured accurately. If your feet vary in size, choose the larger size. Look for shoes that have good arch support, no rough inner seams, at least 1/2” of space between your longest toe and the tip of the shoe, and a structured back to hug your heel. When you find a shoe you are interested in, check to see if it matches your foot shape before you try it on. Place the shoe on top of the outline you brought: if it covers the outline completely, that means it might be a good match. Try the shoe on and walk around to make sure nothing pinches or rubs your foot. For additional tips on finding shoes that are right for your feet, consult with a podiatrist.
It is important to find shoes that fit you properly in order to avoid a variety of different foot problems. For more information about treatment, contact Dr. Joshua David Scoll from Pennsylvania. Our doctor will treat your foot and ankle needs.
Proper Shoe Fitting
Shoes have many different functions. They cushion our body weight, protect our feet, and allow us to safely play sports. You should always make sure that the shoes you wear fit you properly in order to avoid injuries and deformities such as: bunions, corns, calluses, hammertoes, plantar fasciitis, stress fractures, and more. It is important to note that although a certain pair of shoes might be a great fit for someone else, that doesn’t mean they will be a great fit for you. This is why you should always try on shoes before buying them to make sure they are worth the investment. Typically, shoes need to be replaced ever six months to one year of regular use.
Tips for Proper Shoe Fitting
- Select a shoe that is shaped like your foot
- Don’t buy shoes that fit too tight, expecting them to stretch to fit
- Make sure there is enough space (3/8” to ½”) for your longest toe at the end of each shoe when you are standing up
- Walk in the shoes to make sure they fit and feel right
- Don’t select shoes by the size marked inside the shoe, but by how the shoe fits your foot
The shoes you buy should always feel as good as they look. Shoes that fit properly will last longer, feel better, and improve your way of life each day.
If you have any questions, please feel free to contact one of our offices located in Philadelphia, Bensalem, and Fairless Hills, PA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Proper Shoe Fitting
When it comes to maintaining foot health, wearing properly-fitting shoes is important. While wearing the appropriate pair of shoes may seem like a trivial concern, the reality is that improperly fitted shoes cause an astounding amount of injuries to the feet. The overall structure and the biomechanics of our bodies are directly affected by our posture, gait, and feet. Because of this, pain and discomfort felt throughout the body are often related to a problem in the feet. And, most foot problems usually stem from improper footwear.
Shoes should not be purchased with the expectation that they will easily stretch and contort to the size and shape of your feet. When shopping for footwear, look for shoes that fit correctly and comfortably as soon as you put them on. Do not purchase shoes that are too large or that slip in the heel area when you walk. Do not choose shoes that are loose with the intention of wearing thicker socks to compensate for the space. The widest portion of the shoe, the ball of the foot, must be made sure to fit comfortably in the shoe.
Keeping all of these suggestions in mind may be difficult when shopping and when trying to select from a wide array of different shoes. Nonetheless, your time and money will be wasted if you purchase a pair of shoes that are too uncomfortable for you to actually wear them. After finally selecting and purchasing a pair of shoes, try them on at home. To truly ensure whether or not your shoes fit comfortably with normal activity, walk around on a carpeted surface to determine how they feel on your feet.
The possibility of damaging your feet’s 33 joints, 26 bones, and 100+ ligaments is much higher than many people suspect. Finding an appropriate and properly-fitted pair of shoes is perhaps the single most important action you can take to maintain excellent foot health and help prevent injury. The fact that our feet continue to change with age is one that many people often forget. Even if our feet no longer change in size when we mature, our feet will still change in shape.
If you already have pre-existing foot problems, there is a greater possibility that wearing improperly-fitted shoes will worsen those problems. The good news, however, is that appropriate footwear is not difficult to find. While shopping for shoes, remember that improper footwear can detrimentally affect the feet, the entire body and its biomechanical structure as well. The shoes you wear can greatly impact your legs, back, and entire body, as your posture and gait are related to your feet. Finding and selecting the best properly-fitted shoes is necessary in achieving optimal health.
Reminder: When Was the Last Time...?
Should I See a Podiatrist, or Care For Plantar Fasciitis at Home?
Plantar fasciitis, an injury to the ligament that runs along the bottom of the foot, is one of the most frequently diagnosed conditions at the podiatrist’s office. In many cases, conservative treatments are offered to the patient and are typically sufficient for treating the injury. These may include resting and icing the affected foot, wearing more comfortable shoes or orthotics, doing gentle stretching exercises, and taking over-the-counter pain medications. While conservative treatments work for many patients, they aren’t completely effective for everyone. If you have heel pain that is severe enough to stop you from doing your daily activities, gets worse or keeps coming back, or has not improved after two weeks of conservative treatments, it is strongly suggested that you consult with a podiatrist. If you have diabetes, or any tingling or loss of sensation in the foot, it would be wise to seek the care of a podiatrist sooner, rather than later.
Plantar fasciitis is a common foot condition that is often caused by a strain injury. If you are experiencing heel pain or symptoms of plantar fasciitis, contact Dr. Joshua David Scoll from Pennsylvania. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is one of the most common causes of heel pain. The plantar fascia is a ligament that connects your heel to the front of your foot. When this ligament becomes inflamed, plantar fasciitis is the result. If you have plantar fasciitis you will have a stabbing pain that usually occurs with your first steps in the morning. As the day progresses and you walk around more, this pain will start to disappear, but it will return after long periods of standing or sitting.
What Causes Plantar Fasciitis?
- Excessive running
- Having high arches in your feet
- Other foot issues such as flat feet
- Pregnancy (due to the sudden weight gain)
- Being on your feet very often
There are some risk factors that may make you more likely to develop plantar fasciitis compared to others. The condition most commonly affects adults between the ages of 40 and 60. It also tends to affect people who are obese because the extra pounds result in extra stress being placed on the plantar fascia.
Prevention
- Take good care of your feet – Wear shoes that have good arch support and heel cushioning.
- Maintain a healthy weight
- If you are a runner, alternate running with other sports that won’t cause heel pain
There are a variety of treatment options available for plantar fasciitis along with the pain that accompanies it. Additionally, physical therapy is a very important component in the treatment process. It is important that you meet with your podiatrist to determine which treatment option is best for you.
If you have any questions, please feel free to contact one of our offices located in Philadelphia, Bensalem, and Fairless Hills, PA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Plantar Fasciitis
Plantar fasciitis is one of the most common causes of heel pain. The plantar fascia is the thick band of tissue that connects the heel bone to the toes. When this band of connective tissue becomes inflamed, plantar fasciitis occurs. Fortunately, this condition is treatable.
There are several factors that may put you at a greater risk for developing plantar fasciitis. One of the biggest factors is age; plantar fasciitis is common in those between the ages of 40 to 60. People who have jobs that require them to be on their feet are also likely to develop plantar fasciitis. This includes factory workers, teachers, and others who spend a large portion of their day walking around on hard surfaces. Another risk factor is obesity because excess weight can result in extra stress being placed on the plantar fascia.
People with plantar fasciitis often experience a stabbing pain in the heel area. This pain is usually at its worst in the morning, but can also be triggered by periods of standing or sitting. Plantar fasciitis may make it hard to run and walk. It may also make the foot feel stiff and sensitive, which consequently makes walking barefoot difficult.
Treatment for plantar fasciitis depends on the severity of the specific case of the condition. Ice massage applications may be used to reduce pain and inflammation. Physical therapy is often used to treat plantar fasciitis, and this may include stretching exercises. Another treatment option is anti-inflammatory medication, such as ibuprofen.
If you suspect that you have plantar fasciitis, meet with your podiatrist immediately. If left untreated, symptoms may lead to tearing and overstretching of the plantar fascia. The solution is early detection and treatment. Be sure to speak with your podiatrist if you are experiencing heel pain.
What Is Morton's Neuroma?
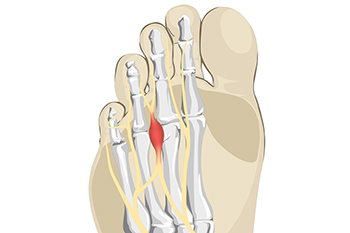 A Morton’s neuroma is the swelling and inflammation of a nerve that occurs between the third and fourth metatarsal bones in the foot. Morton’s neuroma usually causes a burning, stabbing or shooting pain in the ball of the foot and toes because the nerve gets trapped. Wearing tight fitting shoes, like high heels, can play a role in causing this condition, and continuing to wear the shoes can worsen the pain as well. Morton’s neuromas can also cause tingling and numbness in the feet and the feeling of a small stone stuck under the foot. If you think the pain in the ball of your foot that may be a Morton’s neuroma, consulting with a podiatrist for a proper diagnosis and treatment is a good idea.
A Morton’s neuroma is the swelling and inflammation of a nerve that occurs between the third and fourth metatarsal bones in the foot. Morton’s neuroma usually causes a burning, stabbing or shooting pain in the ball of the foot and toes because the nerve gets trapped. Wearing tight fitting shoes, like high heels, can play a role in causing this condition, and continuing to wear the shoes can worsen the pain as well. Morton’s neuromas can also cause tingling and numbness in the feet and the feeling of a small stone stuck under the foot. If you think the pain in the ball of your foot that may be a Morton’s neuroma, consulting with a podiatrist for a proper diagnosis and treatment is a good idea.
Morton’s neuroma is a very uncomfortable condition to live with. If you think you have Morton’s neuroma, contact Dr. Joshua David Scoll of Pennsylvania. Our doctor will attend to all of your foot care needs and answer any of your related questions.
Morton’s Neuroma
Morton's neuroma is a painful foot condition that commonly affects the areas between the second and third or third and fourth toe, although other areas of the foot are also susceptible. Morton’s neuroma is caused by an inflamed nerve in the foot that is being squeezed and aggravated by surrounding bones.
What Increases the Chances of Having Morton’s Neuroma?
- Ill-fitting high heels or shoes that add pressure to the toe or foot
- Jogging, running or any sport that involves constant impact to the foot
- Flat feet, bunions, and any other foot deformities
Morton’s neuroma is a very treatable condition. Orthotics and shoe inserts can often be used to alleviate the pain on the forefront of the feet. In more severe cases, corticosteroids can also be prescribed. In order to figure out the best treatment for your neuroma, it’s recommended to seek the care of a podiatrist who can diagnose your condition and provide different treatment options.
If you have any questions, please feel free to contact one of our offices located in Philadelphia, Bensalem, and Fairless Hills, PA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Morton's Neuroma
A neuroma is a thickening of nerve tissue and can develop throughout the body. In the foot, the most common neuroma is a Morton’s neuroma; this typically forms between the third and fourth toes. The thickening of the nerve is typically caused by compression and irritation of the nerve; this thickening can in turn cause enlargement and, in some cases, nerve damage.
Neuromas can be caused by anything that causes compression or irritation of the nerve. A common cause is wearing shoes with tapered toe boxes or high heels that force the toes into the toe boxes. Physical activities that involve repeated pressure to the foot, such as running or basketball, can also create neuromas. Those with foot deformities, such as bunions, hammertoes, or flatfeet, are more likely to develop the condition.
Symptoms of Morton’s neuroma include tingling, burning, numbness, pain, and the feeling that either something is inside the ball of the foot or that something in one’s shoe or sock is bunched up. Symptoms typically begin gradually and can even go away temporarily by removing one’s shoes or massaging the foot. An increase in the intensity of symptoms correlates with the increasing growth of the neuroma.
Treatment for Morton’s neuroma can vary between patients and the severity of the condition. For mild to moderate cases, padding, icing, orthotics, activity modifications, shoe modifications, medications, and injection therapy may be suggested or prescribed. Patients who have not responded successfully to less invasive treatments may require surgery to properly treat their condition. The severity of your condition will determine the procedure performed and the length of recovery afterwards.
Vascular Testing to Help Determine Peripheral Arterial Disease
Some of the symptoms of peripheral arterial disease (PAD) can include pain, weakness, numbness, loss of hair on your legs, bluish-colored skin on the feet or calves, poor toenail growth, pain or cramps in your legs when walking, and wounds on your feet and legs that are slow to heal. To properly diagnose this vascular condition, your podiatrist may need to know your Ankle Brachial Index (ABI). Simply put, the ABI compares the blood pressure in the arm with the blood pressure in the ankle. Blood pressure during the heart’s contracting/pumping (systolic) phase is slightly higher in the ankle than it is in the arm for healthy people. Determining the ABI is a very simple and non-invasive procedure, using just a blood pressure cuff and a Doppler instrument. The patient lies down and rests for ten minutes. Then, blood pressure is taken at the upper arm, followed by the ankle. The ankle’s blood pressure is then divided by the arm’s blood pressure. An ABI ratio between 1.0 to 1.4 is considered normal. An ABI ratio of 0.9 or less usually indicates PAD—with moderate cases typically ranging between 0.4 to 0.7, and more severe cases falling below 0.4. If you are experiencing any symptoms of PAD, contact a podiatrist right away for a full examination and to see if your ABI should be analyzed.
Vascular testing plays an important part in diagnosing disease like peripheral artery disease. If you have symptoms of peripheral artery disease, or diabetes, consult with Dr. Joshua David Scoll from Pennsylvania. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
What Is Vascular Testing?
Vascular testing checks for how well blood circulation is in the veins and arteries. This is most often done to determine and treat a patient for peripheral artery disease (PAD), stroke, and aneurysms. Podiatrists utilize vascular testing when a patient has symptoms of PAD or if they believe they might. If a patient has diabetes, a podiatrist may determine a vascular test to be prudent to check for poor blood circulation.
How Is it Conducted?
Most forms of vascular testing are non-invasive. Podiatrists will first conduct a visual inspection for any wounds, discoloration, and any abnormal signs prior to a vascular test.
The most common tests include:
- Ankle-Brachial Index (ABI) examination
- Doppler examination
- Pedal pulses
These tests are safe, painless, and easy to do. Once finished, the podiatrist can then provide a diagnosis and the best course for treatment.
If you have any questions, please feel free to contact one of our offices located in Philadelphia, Bensalem, and Fairless Hills, PA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Vascular Testing in Podiatry
In foot care, vascular testing may be required in the diagnosing and treatment of certain podiatric conditions. Vascular testing is particularly relevant for patients with high-risk diabetes, poor circulation, peripheral artery disease (PAD), and chronic venous insufficiency (CVI). Procedures typically involve the examination of blood vessels throughout the body for blockages or buildup.
Vascular testing is very important for the diagnosis of various conditions, including peripheral artery disease and chronic venous insufficiency, as these conditions can greatly affect one’s quality of life and cause pain in the lower limbs. Circulatory problems in the feet and ankles can reflect issues throughout the body, making testing of the blood vessels pertinent.
Testing methods vary between practitioners and can be specific to certain foot and ankle problems. Modern technology has brought about the ability to perform vascular testing using non-invasive methods, such as the cuff-based PADnet testing device. This device records the Ankle-Brachial Index (ABI)/Toe-Brachial Index (TBI) values and Pulse Volume Recording (PVR) waveforms. Contact your podiatrist to determine what vascular testing is available for your needs.